MCO provider rate enhancements in June 22 budget agreement
Thanks to legislative staff colleagues who contributed substantially to this post. This responds to various questions received in recent days.
Background. Historically, California’s managed care organization (MCO) tax has been used to offset General Fund costs for the Medi-Cal program and draw down federal funds. In 2023, the MCO tax was expanded, with a portion of the increased funding proposed for various increased provider reimbursement rates. As shown in Figure 1 of a recent Legislative Analyst’s Office (LAO) report on the Governor’s May Revision proposals, about $300 million of rate increases (labeled as “2024 Medi-Cal rate increases”) were implemented beginning earlier this year. In the May Revision, however, the Governor proposed eliminating planned rate increases of about $2.3 billion to $2.4 billion per year that had been planned to start in 2025 (labeled “2025 Medi-Cal rate increases” in LAO Figure 1). This was one of the largest budget-balancing proposals in the Governor’s May Revision. The legislative budget plan, passed in budget committees on May 30, aimed to restore much of these rate increases, but delayed many of these partial restorations to 2026, to help balance the state budget in 2024-25 and 2025-26.
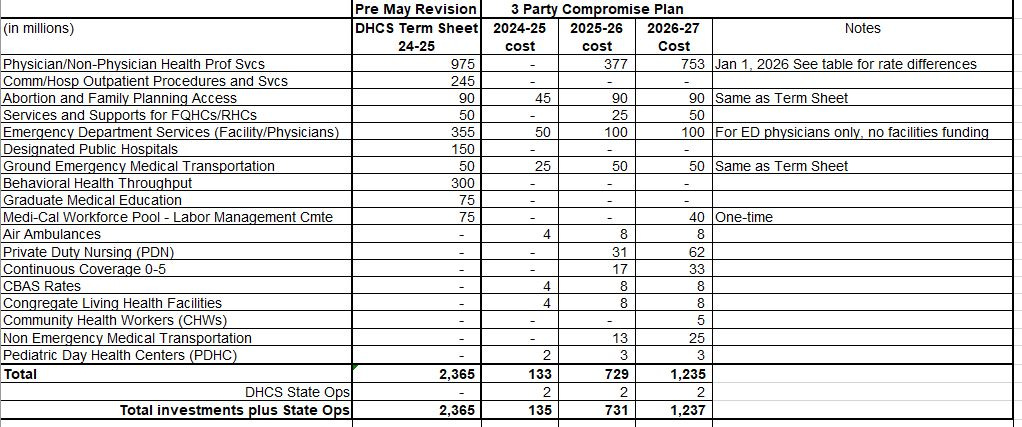
June 22 Agreement Reduces Total Amount of Rate Increases and Redistributes Them. The June 22 budget agreement between the Governor and legislative leaders reduces the previously planned total amount for rate increases, thereby preserving some, but not all, of the Governor’s May Revision budget-balancing proposal. The agreement also redistributes previously planned rate increases, including providing rate increases to some groups not previously slated to receive them and no additional rate increases for some other groups. The plan also funds multiyear continuous Medi-Cal coverage for eligible children aged 0-5 beginning in 2026. The figure below shows the rough full-year costs of the pre-May Revision plan for 2025 Medi-Cal rate increases (labeled “DHCS Term Sheet 24-25”) as well as the year-by-year costs of rate increases and other augmentations in the June 22 budget agreement (labeled “3 Party Compromise Plan”). (DHCS is the state’s Department of Health Care Services.)
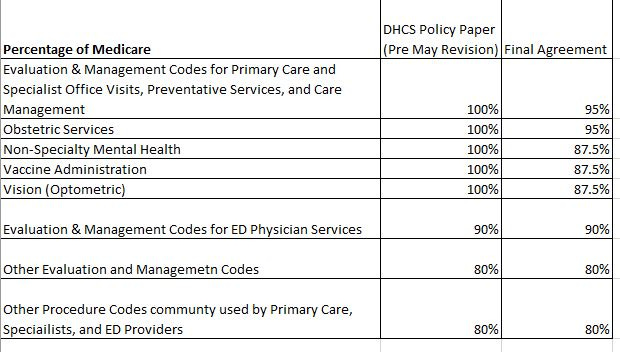
Due to reduced available funding, less funding was provided for primary and specialty care rate increases than planned prior to the May Revision. Moreover, the June 22 budget agreement starts most of these rates on January 1, 2026, one year later than planned—with the exception of Emergency Department physicians, whose increased rates start on January 1, 2025. The table below lists the anticipated rate increases as a “percentage of Medicare.” The “final agreement” column shows the rates for each group in the June 22 budget agreement.
Included in AB/SB 159—Health Budget Trailer Bill. These items in the budget agreement principally are reflected in AB 159/SB 159, the health budget trailer bill. As noted by the Legislative Counsel Digest, various items in this part of the budget agreement would be repealed “if specified provisions relating to the MCO provider tax are approved by the voters at the November 5, 2024, statewide general election.” “If the MCO Tax initiative on the November ballot is approved, the [June 22 budget] agreement provides that this MCO Tax package becomes inoperable, since both cannot be sustained,” the Assembly Budget Committee analysis of SB 159 notes.